Shhh!!! 6 ways to keep the noise down in new and existing hospitals
Hospital executives, healthcare system boards, and clinical staffs have never been more aware of the relationship between noise and patient wellness, says Kurt Rockstroh, FAIA, FACHA, President and CEO of Boston-based Steffian Bradley Architects & Planners. On every one of his firm’s hospital projects, says Rockstroh, “noise reduction is a focus.”
The average noise level in U.S. hospitals has risen from 40 db in the 1960s, to around 70 db today, says Paul Barach, MD, Clinical Professor, Wayne State University. In some hospitals noise levels have been measured as equal to the screeching of a subway train at 200 feet.
The therapeutic merits of good acoustics have been buttressed by several research studies over the past decade, notes physician/architect George Tingwald, MD, AIA, ACHA, who directs Stanford Health Care’s Medical Planning, Facilities Design, and Construction department. That research, he says, has also shown that noise reduction “is a very doable metric.”
ALSO SEE: 7 (more) steps toward a quieter hospital
Stanford has two major construction projects under way in Palo Alto, Calif. Tingwald believes the way a building is built “can change behavior enormously.”
The question, then, is how, and to what extent, design and construction firms can reduce hospital noise and thereby improve clinical outcomes. Opinion varies among the experts.
Noise reduction “has to be more than just applying materials to spaces,” says Tina Larsen, EDAC, AIA, LEED AP, Vice President and Leader of the healthcare studio at Corgan Associates, which joint-ventured with HDR on the 2.1-million-sf, $1.27 billion Parkland Hospital, in Dallas. The 862-bed public hospital is slated to open later this year.
Greg Osecheck, AIA, Associate Vice President with HGA Architects, in Sacramento, Calif., takes a different view. “Hospitals are receptive to ideas, but noise reduction is more on the client and operations side,” he says. His office recently completed Sutter Health’s $281 million Santa Rosa Regional Hospital.
“Hospitals are invested in setting up design standards, but those standards don’t inherently account for all of the issues when you actually move into the building,” adds Josh Cushner, an Associate Principal with Arup, whose SoundLab studio, in San Francisco, addresses that problem by simulating building acoustics during design.
David Sykes, Chairman of the Acoustics Research Council, asserts that noise reduction strategies must still contend with the inclination of some hospitals to organize their operations around staff needs rather than patient needs. The proliferation of machines and monitoring devices, with all their buzzes, beeps, and alarms, increases the cacophony of hospital soundscapes, he says.
Here are six effective noise- and vibration-reducing strategies, based upon the advice of 20 experts consulted for this report.
1. Start with a full assessment of the exterior environment.
To understand what the façade needs to do to keep out noise, Building Teams must account for noise generated by cooling towers, ambulance/emergency centers, helipads, and the urban surroundings. “Mitigation often demands a lot from curtain walls,” says Kenneth Van Wyk, President, Acoustics by Design, an independent acoustics consulting firm.
Site logistics must also be taken into account. Dallas’s new Parkland Hospital is located in a high-traffic area, adjacent to a multi-lane highway and train station. “We wanted to pull the entrance away to a more peaceful environment,” says Corgan’s Larsen. The design team of Corgan and HDR moved the entryway of the 862-bed public hospital to a quieter setting in a newly created one-acre park, thereby “putting the park back in Parkland.”
2. Fortify partition designs, and reduce or eliminate penetrations through walls.
Beefing up floor-to-ceiling partitions prevents sound from seeping into patient rooms. “It’s really important to have well-constructed partitions,” says Jamie Huffcut, Health and Wellness Workplace Strategist in Gensler’s Washington, D.C., office.
Building Teams are specifying acoustical materials for ceilings, walls, and partitions with higher sound transmission class ratings. (The higher the STC, the better.) “I haven’t worked on a hospital in a while that didn’t use sound-limiting ceilings,” says David Scott, Operations Manager with project management firm Faithful+Gould. Scott says he’s also seeing more coffered ceilings and sound-absorbing panels in hospital rooms and public spaces.
Robert Gambrell, Senior Vice President with Robins & Morton, says using thicker drywall and acoustical caulking, which have a higher sound transmission class, can reduce noise transmission.
Eliminating wall penetrations also helps reduce noise transmission. Traditional rooms with shared headwalls can have as many as 40 penetrations going through a wall. Robins & Morton completed MaineGeneral’s $224 million, 640,000-sf Alfond Center for Health, in Augusta, Maine, with 192 single-bed patient rooms that don’t share headwalls. Eliminating shared headwalls reduced the number of penetrations and the resultant noise infiltration in patient rooms.
3. Reduce sound transmission from mechanical systems.
Acoustics by Design’s Van Wyk recommends locating HVAC and other mechanical equipment as far from patients as possible. Mechanical equipment should be properly mounted to reduce vibration. Fans and coils should not be installed in patient rooms, says Van Wyk.
Early planning and participation are essential. “You need to get in at the early stages to perform baseline studies” to determine vibration levels, says Alan Oldfield, MEng, CEng (UK), PEng, Senior Acoustics Engineer with AECOM, in Mississauga, Ont.
“I don’t care what the building looks like. I care what the building does.” —Jean Elrick, MD, Massachusetts General Hospital
For Massachusetts General Hospital’s Lunder Building, in Boston, NBBJ located the mechanicals on the fifth floor (of 10 above-ground stories), above the operating rooms (“big energy guzzlers,” says NBBJ’s Susan Markovitz, AIA, Principal and Lead Medical Planner) but below ICU, neuroscience, and cancer units that needed more quiet. NBBJ also had to keep mechanical vibrations from negatively affecting an inter-operational MRI suite that Mass General asked for late in the design process.
Gensler’s Huffcut notes that some new HVAC systems are so quiet that “you lose some of the white noise” common in many older hospitals. Hospital designers have been experimenting with white noise machines, which create a slight buzz that masks more disruptive noises. A word of caution: Installing white noise machines in patient rooms can make it hard for patients and others in the room to decipher speech.
4. Separate patients from sources of noise.
Commotion emanating from nursing stations, especially during nighttime shift changes, is often cited as a big reason why patients can’t sleep.
One popular solution has been to decentralize workstations away from patient rooms. In more-sensitive care areas, some hospitals have installed small glass-enclosed nurse stations between two patient rooms. Bonny Slater, ASID, Gensler’s Senior Interior Designer, Health & Wellness, says she is seeing smaller centralized workstations with space for fewer nurses and, theoretically at least, less racket.
The drawback is that decentralization approaches can limit the clinical staff’s ability to communicate at critical moments. “You need someplace where specialists can speak together,” says Slater.
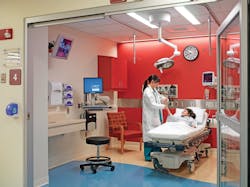
Patient rooms have gotten much larger and may incorporate areas where clinical staffs can convene; some even have space for patients’ family members and visitors, all of which can add up to more noise. For Mass General’s Lunder Building, NBBJ and manufacturer Horton Automatics developed a system of sliding glass doors that allows patients’ rooms to be closed off but still provides sight lines for staff to see patients.
Hospitals are also being designed to separate so-called “on-stage” activities (those related directly to patient care) from noisier “off-stage” activities (housecleaning, transport, food service, etc.). Steve Evers, President of TRO JB, MaineGeneral’s architect, says this strategy is not unlike how Disney keeps support activities out of sight of visitors to its theme parks.
In its design for the 640,000-sf Baystate Medical Center, in Springfield, Mass., Steffian Bradley positioned vertical circulation and public spaces away from patient rooms. Noisy equipment was stowed in off-stage zones. Rockstroh says the hospital has been getting increasingly higher patient satisfaction scores. “Some of the staff said it was too quiet,” he says.
At Mass General’s Lunder Building, elevators, waiting rooms, and staff rooms are set along the circulation spine. Patient rooms are staggered in a sawtooth pattern to attenuate sound and provide a smidgen more privacy. “We understand the idealized workflow of our staff, and the building is designed to complement that workflow,” says Jean Elrick, MD, Mass General’s Senior Vice President of Administration. “I don’t care what the building looks like; I care what the building does.”
5. Check out the latest sound-absorbing materials and acoustical products.
Hospitals and their Building Teams need to embrace sound-absorbing materials, says Acoustics by Design’s Van Wyk.
Gary Madaras, PhD, Associate AIA, ASA, INCE, an acoustics specialist with ceilings manufacturer Rockfon, notes that a 2008 white paper from the Center for Health Design and the Georgia Institute of Technology (http://bit.ly/1egDTjW) recommended installing high-performance sound-absorbing ceiling tiles as one of eight design interventions that any hospital can take.
The use of sound-absorbing materials in hospitals is relatively new. Older hospitals were almost always built with hard interior surfaces that could be easily maintained. Sound ricochets off of these surfaces, making those hospitals all the louder.
Infection control is an important reason why certain acoustical materials have been kept out of hospitals. “Fluffy surfaces aren’t conducive to hygiene,” says AECOM’s Oldfield, which is why some insulation products don’t make the specifications cut.
The Facilities Guidelines Institute’s latest guidelines state that healthcare designers should consider the extent to which a material can be cleaned, washed, painted over, and maintained when specifying sound-absorbing materials.
Architects and their hospital clients are getting more comfortable with using acoustic materials for walls, ceilings, and floors. Van Wyk says he’d like to see more carpeting in waiting and reception areas, and even on some corridors. Rubber flooring, which is more forgiving on nurses’ feet, can be a “good compromise,” he states. All the flooring in Mass General’ Lunder Building—which was a test site for FGI’s 2010 guidelines—is rubberized. The new Parkland Hospital will have 750,000 sf of rubber flooring.
Corgan’s Larsen says acoustical ceilings were “an important factor” in attenuating sound bouncing off the stone walls and floors in Parkland’s three-story entrance and lobby. The Lunder Building used sound-absorbing materials on its walls, says NBBJ’s Markovitz.
6. Minimize “alarm fatigue.”
Alarm noise is among the top reasons why hospital patients can’t sleep. Up to 95% of alarms don’t require a clinical response. Many alarms give off false-positive alerts due to improperly applied sensors, badly maintained equipment, and poor staff training.
“Alarm fatigue” has become serious enough that the nonprofit ECRI Institute—whose goal is to bring applied science disciplines to healthcare operations—and the Joint Commission, which accredits healthcare organizations, say it is among the worst technology hazards in hospitals.
The Joint Commission wants hospitals to establish policies and procedures for managing alarms and educating their staffs about alarm systems by January 1. To fight the “decibel war” being waged in hospitals, Doug Erickson, CEO of the Facilities Guidelines Institute, says he expects FGI’s 2018 revised guidelines to chime in more specifically about alarm control.
Barach, whose specialty is alarm fatigue, says the healthcare industry is still in the early stages of installing customized alert systems. NBBJ’s Marovitz says she’d like to see alarms replaced with “visuals” like light panels outside of patients’ rooms.
Virtually everyone in the healthcare field can’t wait for the day when hospitals finally kiss good-bye to blaring intercom systems in all but life-saving areas. “Overhead PAs are going away,” says Corgan’s Larsen.
Less-obtrusive products are already emerging. Holosonics’ Audio Spotlight, a directional loudspeaker system, uses a beam of ultrasound as a “virtual acoustic source” to control sound distribution.
Hospitals are also reassessing the relative value of different alarms in their operations. TRO JB’s Evers says he sees more caregivers armed with mobile devices that can receive alarm signals sent from patients’ rooms.
That’s the case at the $300 million Baystate Medical Center in Springfield, Mass. Most of Baystate’s nurses carry personal devices so that “physio alarms go directly to them,” says Lou Faassen, the hospital’s Manager of Construction Services.
The 150-bed Lunder Building uses smartphone technology from Voalte, a text-messaging and personal alarm system that links physicians, nurses, lab technicians, and transport teams. This system distinguishes alarms in a range from urgent to less important, so staff members can respond appropriately. “This has been quite an important advance for us,” says Mass General’s Elrick.
Hospitals must also train their staffs to overcome alarm fatigue. While there isn’t a one-size-fits-all standard for minimizing alarms, it can be done. Boston Medical Center recently implemented a six-week pilot program that took a cost-effective approach, and saw a drastic drop in audible alarms. New technologies allow alarms to be customized for different levels of crisis alert, says Chris Kay, ACHE, Managing Principal–National Healthcare & Science Buildings Practice at Jacobs.
still PLENTY OF ROOM FOR IMPROVEMENT in america’s hospitals
With Obamacare imposing tougher performance requirements for accreditation, insurance reimbursement, and patient readmission, hospitals can find themselves chasing the unattainable: silence. That may be unrealistic, say AEC officials, but they still insist there’s plenty of room for improvement in new and older hospitals to turn down the volume.
Tingwald says that Stanford Health Care’s hospitals are engaged in a “quiet hospital initiative” that relies on better acoustical design and materials but also addresses how the staff interacts with patients. When nurses dispense medication, they turn on small lights attached to their uniforms, which indicate they should not be disturbed. TVs in reception areas are not allowed to be blaringly loud.
There are new products coming onto the market that are helping hospitals reduce their noise levels. Cushner says Arup—which has numbered Yale Health Services and Kaiser Permanente among its clients—is looking into micro-perforated wood and steel products that could be used as acoustical panels.
Materials are only part of the solution, says Cushner: “The harder job is creating the willingness within the industry to make changes.” He advocates for early planning and strategy studies to produce data that can inform the direction of a new build or renovation project.
“These studies need to take into account the hard and soft issues of noise,” says Cushner. “They need to happen before pen goes to paper.”