Never waste a crisis
Count Fred Bland among the AEC executives who were blown away by how efficiently their associates performed from home during the pandemic lockdown. “It was a great surprise to me that, remotely, we’ve been able to serve our clients well,” says Bland, FAIA, AICP, Managing Partner with Beyer Blinder Belle. He attributed that success to a combination of technology and esprit de corps.
Lou Cornell, CEO of WSP USA, says that “shock is not an overstatement” to describe his amazement at how proficiently his company functioned with 90% of its 10,000 employees out of their offices. “Our people embraced this, and it can only benefit us down the road.”
Working remotely, it turns out, was an eye-opener for AEC firms during the pandemic that seemed to dispel a number of preconceived notions. Firms and their clients are now pondering their office densities and real estate portfolios. The coronavirus raised concerns about whether a building’s airtightness is inimical to infection control; whether resilience on all fronts needs far more attention and investment; even whether the U.S. still had a corner on problem-solving for the built environment.
Firms are now taking a broader perspective. “We will look at any project with the lens of safety and infection control,” says Tatiana Guimaraes, Associate Principal with Perkins and Will. “If we were to design a school today, perhaps we should consider the ability for a classroom to be a four- to six-bed patient unit.”
“Right now, all bets are off as to what ‘evidence-based design’ actually means,” says Deborah Wingler, PhD, Vice President and Health Research Lead with HKS. “We can’t wait for science to be perfect. We need to let go of barriers to entry that hold up innovation.”
HOK documented everything it did during the pandemic’s rage, “so we could learn every day,” says Thomas Quigley, AIA, LEED AP, Director of Healthcare and Senior Principal with HOK. The firm’s healthcare group includes a consulting practice whose Chief Medical Officer, Andrew M. Ibrahim, MD, is a surgeon affiliated with the University of Michigan. The practice also includes Senior Healthcare Consultant Kathleen Schwarz, MPA, BSN, RN, a registered nurse who worked 12-hour shifts in the ICU at New York Presbyterian Hospital during the crisis.
The Boldt Company, taking its cue from how hospitals in Asia manage incoming patients during peak periods, installed tent triage units in the parking lots of the 26 hospitals in the Advocate/Aurora healthcare system within three weeks.
“We do a lot of strategic planning to help healthcare systems rationalize their capabilities, and this crisis will inform our future designs,” says Quigley. Ibrahim predicted that healthcare will undergo “a fundamental redesign centered around flexibility.”
Several firms in search of new ideas cast their nets wider during the pandemic. “The crisis opened a lot of people’s eyes,” says Jeffrey Brand, AIA, EDAC, National Healthcare Leader with Perkins Eastman. The firm, with help from healthcare clients in Hong Kong, has been analyzing a state-of-the-art facility for infection control, medical surges, and beds that can be converted to ICUs.
Woods Bagot drew insights from China where, even after Beijing loosened its quarantine, 90% of meetings at the firm’s studio there were conducted via video conference. “Everyone wears a face mask, even on Zoom calls,” wrote Stephen Jones, the firm’s Director-Regional Managing Chair China.
HDR took cues from how China and South Korea managed patients entering healthcare facilities. Hank Adams, AIA, FACHA, EDAC, HDR’s Global Director of Health, notes that almost all emergency departments in China include a buffer zone with a triage area. That concept informed HDR’s design of tent structures for the Advocate/Aurora healthcare systems in Illinois. The Boldt Company installed those tents in the parking lots of that system’s 26 hospitals in less than three weeks. Adams predicts that this solution will become more common in the U.S.
From its work in Haiti and Liberia, MASS Design Group has learned that “first-world solutions aren’t always the only answer,” says Chris Scovel, RA, LEED AP, the firm’s Director. Its experiences overseas guided MASS Design’s consultation with Boston Healthcare for the Homeless for a project in Boston’s South End that put up two temporary 1,600-sf tents with bathrooms and space for 40 beds, to isolate COVID-19 infected homeless people.
MASS Design also released guidelines for limiting contagion in COVID-19 tent clinics, focusing on increasing airflow and controlling patient flow (bit.ly/3aObr6e).
“The conventional wisdom has always been that the only way to deliver healthcare was within a sophisticated high-tech environment. We’ve since discovered that you can do a lot with a whole lot less,” observes HOK’s Quigley. He points specifically to the Army Corps of Engineers’ “scalable approach” to managing surge capacity as one replicable model. “We’ve been designing around those principles.”
If nothing else, the COVID-19 crisis tested the industry’s ability to respond quickly. DLR Group’s design for temporary Assessment and Recovery Centers in King County, Wash., whose goal was to provide 2,500 clinical beds, first and foremost had to answer the question: What materials and equipment are available in two weeks?, recalls Lori Coppenrath, LEED AP, DLR Group’s Justice and Civic Planner.
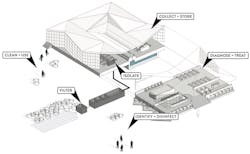
Temporary healthcare additions could become common post-coronavirus
Ennead Architects was involved in the design of a 14-bed tent for lower-acuity patients that, if used, could expand NYU Langone Health’s emergency department. David Tepper, AIA, Principal and Healthcare Practice Leader with Ennead, has also heard some institutions talking about enlarging hospital rooms so they could accommodate a second bed during surges.
The irony, says Tepper, is that the trend over the past several years has been to reduce hospital beds and to move patients to outpatient clinics. “But how close to the bone can you cut that number?” he asks.
Just how will healthcare systems handle patient overflows in the future? Tepper believes one solution could be to set up ambulatory clinics so they can perform more procedures.
‘Right now, all bets are off as to what evidence-based design actually means. We can’t wait for science to be perfect. We need to let go of barriers to entry that hold up innovation.’
— Deborah Wingler, PhD, HKS
AECOM has been recommending that hospitals include semi-permanent structures that allow them to ramp up their surge capacities. The firm worked with the Army Corps of Engineers to build large temporary alternate patient care facilities in New York, Colorado, and Tennessee, including a 1,024-bed unit on Long Island, N.Y., that originally was going to be for non-COVID 19 patients but ended up devoting 80% of its beds to the infected.
Karl Jensen, Executive Vice President–National Government Practice for AECOM’s Design and Consulting Services–Americas, posits that temporary structures could be repurposed for other functions during more normal periods.
And while COVID-19 is not an airborne virus, hospitals should be asking themselves how to prepare for the next pandemic that might be. “It seems to me that we should be discussing all possibilities,” says John Pappas, PE, LEEP AP, Principal and Mechanical Engineer with Mazzetti. The MEP engineering firm is currently working on an emergency department expansion in Georgia, “and I know part of that design conversation will be about converting to 100% outside air and 100% exhaust, which would be expensive, but…,” says Pappas.
Less density will be in demand
Lessons learned during the coronavirus haven’t been confined to healthcare.
Kinder Baumgardner is Managing Principal with SWA Group, a landscape architect in Houston. He noticed that programmed common spaces such as the Avenita district near his city’s convention center, which are usually packed with people, were virtually empty during the pandemic lockdown. In contrast, unprogrammed spaces, like Buffalo Bayou Greenways and Parks in Houston, which includes 150 miles of trails that traverse the city, were brimming with users. Baumgardner concluded that, going forward, unprogrammed space might be what neighborhoods and communities embrace. And programmed spaces, which are designed to attract hordes of people, might need to be rethought for less density.
Sam Nunes, AIA, LEED AP, Founding Partner with WRNS Studio, pointed out that for the past 20 years, firms like his have been designing office buildings to densify their floor plates for group productivity. But if working remotely catches on in a big way after the coronavirus subsides, “that could change, and more collaboration could go online.”
Theoretically, a shift like that would leave more room for social distancing. But it could also leave office tenants will a lot of unused space they’re paying for. WSP USA has about $250 million in real estate value. “Do we need all of that if remote work is viable,” asked Tom Lewis, PE, President and CEO, and President of Federal Programs and Logistics?