Designing a health facility for the next pandemic
Eppstein Uhen Architects (EUA) has released a 16-page guide that provides pandemic considerations for health facility design. The document focuses on four objectives:
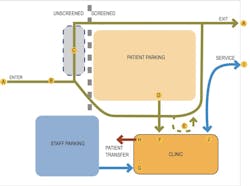
1. Reducing patient presentations at facilities, with specific focuses on telehealth, site design and planning, and drive-through testing. For example, the guide’s considerations for reducing patient presentations include using the facility’s parking lot to manage who enters the building. It recommends a single point of entry and exit, a staffed gatehouse to direct and track patients (via smartphone technology), and drive-through services for pharmacies and labs.
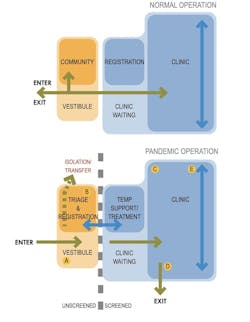
2. Isolating infectious patients, and how to prepare vestibules, entries, waiting rooms, and reception areas. The guide recommends larger vestibules to accommodate more functions and equipment, as well as temperature screening, physical distancing, and touchless entry supplemented by hand sanitizer stations and mask dispensers. Planning, the guide states, will also consider “placing a negative pressure multipurpose room adjacent to registration to isolate patients with symptoms of infectious diseases.
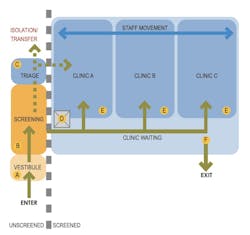
3. Improving facilities’ ability to reduce the spread of infection. The guide makes specific planning recommendations for clinics, hospital lobbies, emergency departments, elevators, materials management, and restrooms. Triage areas at the front door will help sort well and unwell patients. One-way patient flow will ensure patients don’t cross paths with potentially unwell patients who are entering the building.
For clinics, EUA favors a “library” model that includes community spaces (e.g., rooms for meetings and group therapies, physical therapy, or for staff break rooms) with access to the building’s main entrance. During a pandemic, a community space would be converted to serve as a buffer between screened and unscreened patients.
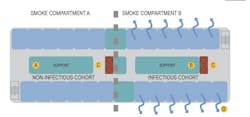
4. Providing surge capacity for high-volume episodes. The guide offers considerations for separating infected patients, providing separate entrances, ventilation (including providing a negative pressure relationship in the infectious side of the unit), and repurposing lower-acuity patient care spaces for increased patient beds.
“Planning a building that seeks to fully address all aspects of operations during a pandemic is a major undertaking,” the guide concedes. Therefore, “it is important to be intentional about the decisions each organization makes around pandemic planning for each project.”