Process mapping simplifies healthcare design
Healthcare design is a complicated, iterative process of back-and-forth communication between stakeholders and the design team. The first step is understanding the purpose of the building or space to be designed and the processes it will accommodate. As designers and trusted advisors, we aim to get at the heart of the issues our clients want to solve. One method that helps us achieve that is called process mapping, a way of tailoring design solutions to specific problems by visualizing every step in an organization’s existing or proposed processes.
What is Process Mapping?
Process mapping is a relatively simple exercise for uncovering the root causes of issues that, in some cases, our clients don’t even know about yet. First we chart the course through an organization’s current procedures. Then we highlight opportunities to improve the experience and outcomes for patients, staff and the facility as a whole. When it’s done right, the maps created contain enough information to develop simulations of various design alternatives. The ability to run simulations off a process diagram is not universal, however. The diagram must be constructed in the right way and answer the right questions.
Perhaps the greatest benefit of process mapping in healthcare is in finding opportunities to add value. This could mean mapping how patients move through a specific episode of care like total joint replacement. Consider those patients’ path from referral to discharge. How cumbersome is that process? Is it easy to navigate or unnecessarily complicated? Can a design solution alleviate front-end issues during the check-in process? How can we facilitate the patients’ journey and improve their experience so they continue through post-acute care for full rehabilitation?
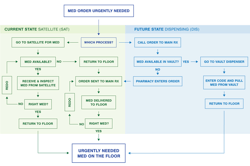
In the example illustrated above, the “current state” map in green shows how urgently needed medication is distributed in a hospital tower with satellite distribution components on every third floor. The “future state” map in blue represents a proposal to install medication dispensers on every floor.
The new model would clearly reduce the time staff spend traveling to and from satellite dispensers only to return empty handed. But rather than undertaking a major renovation, the client might prefer to keep its existing model while increasing the amount of medication in stock at each satellite dispenser.
By simulating both scenarios, we can learn which alternative will add more value for the hospital and its patients and staff.
Adding Value with Process Mapping
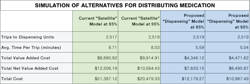
The next chart shows the results of that simulation. What we find is that increasing the availability of medications at existing satellite locations from 85% to 95% does save money by increasing staff efficiency and utilization. Providing dispensing units at each floor, however, would cut the cost associated with distributing medication almost in half! Those savings grow even larger when availability increases from 85% to 95%.
Process mapping allowed us to identify the source of inefficiency, develop multiple potential solutions, and simulate their implementation to determine the real value of one solution over another. “Value,” of course, can mean different things to different clients. In this scenario, value was the money saved by reducing inefficiency in the distribution of medication. For another hospital, it might mean reducing the backlog of patients and wait times in an Emergency Department.
Collaboration is Key to Process Mapping and Simulation
Successfully uncovering problems, determining their magnitude, and pinpointing when and where they arise requires a collaborative effort between the people most familiar with a given process. Fortunately, process mapping is a great way to bring multidisciplinary stakeholders to the table to determine the origin of a problem and find a solution that’s easy for everyone to visualize and understand.
Sometimes the answer is as simple as removing steps that contribute little or no value. Sometimes it’s more complicated. But the only way to find out is to go through the process!
About the Author: Ray is an architect and project coordinator in GS&P’s Healthcare market. He is an EDAC certified professional and LEED Green Associate with more than 13 years of architectural experience, seven of which are healthcare-specific. In addition to his professional contributions to the healthcare architecture field, Ray also enjoys photography, running and visits to local museums with his young son, Sebastian.
About the Author
Gresham Smith
The Gresham Smith blog is about starting discussions. We want to get people thinking about issues and trends that are impacting the design services industry and the market sectors Gresham Smith architects, engineers, interior designers, planners, consultants and environmental scientists serve. Great ideas are typically enhanced through conversation and often stifled by singular views and opinion. We hope you'll join in this conversation and help us to create a meaningful dialogue. Follow us on Facebook, Instagram, LinkedIn, Twitter, Vimeo, and YouTube.