Design solutions for mental health as a secondary diagnosis
In the middle of a mental health crisis, with a healthcare system that does not fully support the wide variety of psychiatric needs, hospital leaders and designers took their experience, perspectives, and creativity, rolled up their sleeves, and got to work to reconsider how patients with mental health needs could be best cared for. How then, can hospital workflows and departments be equipped to treat these patients? Two creative solutions were presented in the “Mind the Gap” session at the 2022 Healthcare Design Conference.
Complexity Intervention Units
Today’s patient populations are more complex than ever and are being admitted with primary and secondary diagnoses. The frequency in which one co-occurrence is a behavioral health issue led Froedtert Medical Center to create what they term a Complexity Intervention Unit (CIU). This is a department dedicated to patients presenting with a medical primary diagnosis but who have a secondary behavioral health diagnosis. For example, this could be a patient admitted for diabetic complications who also has schizophrenia.
The CIU has dedicated nursing staff specially trained for various workflows. The team of providers is built around the patient population, with physicians dual certified in behavioral health and internal medicine, for example.
The CIU team serves as a Behavioral Intervention Response Team (BIRT) throughout the hospital, performing consults as a proactive tool for better patient outcomes. The department is licensed as a Medical Unit—not a Psychiatric Unit. Rooms are designed to be safer than a standard hospital room, but not as stringent as a Behavioral Health care unit. The CIU at Froedtert Medical Center provides concurrent care for medical and mental diagnosis. This reduces the patient stay and readmissions.
Other units within the hospital are relieved from the demands of concurrent mental health diagnosis—challenges which they are not always properly trained to handle. This is one example of a creative process and workflow to address the complex challenges of care for patient mental health in hospitals.
Behavioral-Friendly Rooms
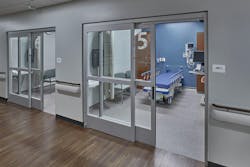
Boston Children’s Hospital approached the demand for flexibility of access for co-occurring diagnosis another way. Rather than dedicating an entire unit, they have woven the space into existing units. Except for the ICU, each department has at least one behavioral-friendly room. This is a room designed to look like other rooms on the floor but integrates a level of safety for patients with a secondary mental health diagnosis.
The Behavioral Intervention Response Team goes to the units to provide specialty mental health care. Staff respite areas on every unit provide space for the BIRT and unit staff to connect. The patient rooms swing as regular rooms when the patient load demands it.
Years ago, the available anti-ligature products would make these rooms look and feel much different than a typical room. The pressure for non-institutional ligature resistant products has driven creativity in the industry, and we will continue to see marked improvements. With the goal of having behavioral-friendly rooms like regular patient rooms—this practice could be adopted universally. All patient rooms could have a higher level of safety. The care for co-occurring mental health conditions at Boston Children’s Hospital is incorporated into departments, and the workflows support this integration.
The healthcare system does not clearly address the frequency or nuances of patients with mental health needs.
Hospital staff understand that psychiatric episodes happen across all departments, and patients presenting with a medical diagnosis often have co-occurring behavioral conditions. Having the space, the team, and the workflow to properly care for the mental health of all patients creates better outcomes for the health of our communities.
With one in five Americans suffering from a mental illness each year, the demand is high. Froedtert Medical Center and Boston Children’s Hospital established two ways to treat the complexity of todays mental health needs.
About the Author
Design Collaborative
Design Collaborative is an award-winning multi-disciplinary design firm founded in 1992, with the belief that through our work, we can improve people's worlds. With nationally recognized expertise and a passion for improving worlds, DC has grown to become consistently ranked amongst the top 100 firms in the country by staying focused on designing people-first places. At DC, we provide boutique firm experience with big firm expertise and resources. Our team includes architects, engineers, interior designers, cost estimators, graphic designers, and support staff. We are a one-stop solution, providing real-time collaboration and problem-solving. Follow Design Collaborative on Facebook, Instagram, and LinkedIn.