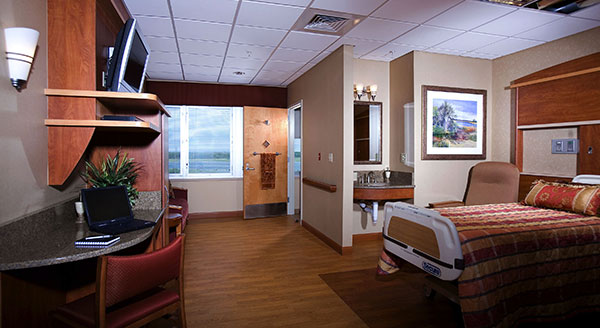
As human beings, we cannot always control the timing and severity of illnesses, but as healthcare designers, we do have some control over the environment in which chronically or terminally ill patients spend their days.
Palliative care strives to make patients comfortable as they are receiving treatment for a severe illness. It is an important part of end-of-life or hospice care, but, as this New York Times article points out, palliative care can also play an integral role in speeding recovery and preventing chronic illness.
As hospitals seek to avoid Affordable Care Act penalties for poor patient satisfaction, many expect the palliative care field to grow quickly. Even before the ACA, the number of palliative care programs among American hospitals with 50 or more beds increased by approximately 125% from 2000 to 2008. The number of people dying in such facilities is also rising; though 70-90% of people say that they would prefer to die at home, approximately 75% die in hospitals or nursing homes.
More attention is being paid to the design of palliative care facilities, and a growing body of evidence is supporting the development of proven design strategies to address the four areas of pain experienced by severely ill patients- physical pain, psychological pain, social pain and spiritual pain.
Create a Homelike Space
When patients move into a palliative care facility, they surrender much of the control that they are used to in their homes and enter a medicalized environment that some perceive negatively. Changing this perception could require a shift in viewpoint for hospital administrators, staff and patients.
As one essay points out, "The idea of a hospital being an honoured place with dying patients as honoured guests opens a new window into our daily reality of working in hospitals" (Donnelly, 2013). In hospitals and in independent palliative care facilities, even small changes- such as the location of the clock or a bedside lamp- can create a less institutional, more homelike environment that empowers patients, relieves stress and improves perceptions of care. Best practices to consider include:
- Allow patients to control environmental factors such as the temperature of their room and the channels playing on their television.
- Help patients to mimic homelike activities by including kitchens with spaces for families to prepare meals and eat together and sitting rooms or gardens for groups to gather.
- Mitigate external noise with strategic layouts and noise absorptive finishes. Studies have shown that, while patients do not always enjoy environments that are "too quiet", they dislike noise disturbances outside of their room or family, such as other patients' televisions or staff conversations. The layout of nursing stations, staff lounges and other heavily trafficked spaces should be designed to concentrate noisy activity in specific areas.
- Designers should consider that patients have an average of 5.7 objects with them near their bedside when they enter palliative facilities and provide space for keeping these mementos nearby.
- Provide plenty of natural light and nature views. In interior corridors, feature artwork depicting natural scenes.
Balance Private and Social Spaces
There is no one formula for patient privacy in the palliative setting- different patients prefer different levels of privacy and social interaction. In one study, the majority of patients expressed a strong preference for multi-bed rooms while they were feeling well enough to interact, and single rooms when they were very ill or dying.
In another study, the need for privacy was ranked much higher by family members than by patients themselves, indicating that families need space for confidential discussions and often want to be alone with their loved one. Additionally, studies highlight the importance of chapels and other spaces for private reflection, both for patients and for their families. Taken as a whole, research suggests a need for a mix of multi- and single-bedded rooms, as well as a mix of public lounges with other semi-private and private spaces.
Staff Support
As important as the physical environment is, staff behavior can make or break the palliative care experience. Providing an environment that supports staff needs will translate to better care for patients, as well as higher staff satisfaction and retention rates. In palliative care facilities, staff complaints often center on layout.
Many report having to walk long distances and also express concerns about being able to adequately monitor patients, especially at night. Other worries include small patient rooms inefficient for clinical tasks, lack of family space, and lack of privacy for bereaved families. To alleviate concerns, designers should work with staff early in the planning process to develop a layout that minimizes staff footsteps and provides adequately sized patient, staff and family zones.
With these best practices, designers can create spaces that provide patients with comfort and dignity while still supporting state-of-the-art care. Doing so, they can become an important part of the team and professionals and caregivers that aims, as compassionately as possible, to ease the pain of severe and terminal illness.
Read more posts from the GS&P Dialogue blog.
About the Author
Sheila J. Bosch, PhD, EDAC, LEED AP, serves GS&P as a director of research. In this role she is a firmwide resource supporting the firm's ability to more extensively understand and apply research evidence regarding how the physical healthcare facility environment can improve patient and staff outcomes, such as reducing falls and improving patient satisfaction, and to contribute to this important and growing body of knowledge.
Studies consulted for this post:
2002-2010 American Hospital Association Annual Hospital Surveys for FY 2000 to 2008; and Data from the Center to Advance Palliative Care (CAPC) 2009 National Palliative Care Registry.
Brereton, L, Gardiner, C., Gott, M., Ingleton, C., Barnes, S. & Carroll, C. (2011). The hospital environment for end of life care of older adults and their families: An integrative review. Journal of Advanced Nursing. http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2648.2011.05900.x/abstract
Cordts, G.A. (2007). Palliative care in the care of patients with cancer. Johns Hopkins Bloomberg School of Public Health. Presentation accessed online on October 23, 2013. http://ocw.jhsph.edu/courses/fundonc/PDFs/Lecture6.pdf
Donnelly, S. (2013). Patient dying in hospital: An honored guest in an honoured place?. Q.J. Med, 106:697-700.
Rigby, J., Payne, S. & Froggatt, K. (2010). What evidence is there about the specific environmental needs of older people who are near the end of life and are cared for in hospices or similar institutions? A literature review. Palliative Medicine, 24(3):268-285. http://ocw.jhsph.edu/courses/fundonc/PDFs/Lecture6.pdf
Rowlands, J. (2008). How does the environment impact on the quality of life of advanced cancer patients? A qualitative study with implications for ward design. Palliative Medicine, 22:768-774. http://pmj.sagepub.com/content/22/6/768.abstract
More from Author
Gresham Smith | Aug 17, 2023
How to design for adaptive reuse: Don’t reinvent the wheel
Gresham Smith demonstrates the opportunities of adaptive reuse, specifically reusing empty big-box retail and malls, many of which sit unused or underutilized across the country.
Gresham Smith | May 24, 2023
Designing spaces that promote enrollment
Alyson Mandeville, Higher Education Practice Leader, argues that colleges and universities need to shift their business model—with the help of designers.
Gresham Smith | Apr 24, 2023
Smart savings: Commissioning for the hybrid workplace
Joe Crowe, Senior Mechanical Engineer, Gresham Smith, shares smart savings tips for facility managers and building owners of hybrid workplaces.
Gresham Smith | Mar 20, 2023
3 ways prefabrication doubles as a sustainability strategy
Corie Baker, AIA, shares three modular Gresham Smith projects that found sustainability benefits from the use of prefabrication.
Gresham Smith | Jan 19, 2023
Maximizing access for everyone: A closer look at universal design in healthcare facilities
Maria Sanchez, Interior Designer at Gresham Smith, shares how universal design bolsters empathy and equity in healthcare facilities.
Gresham Smith | Dec 20, 2022
Designing for a first-in-the-world proton therapy cancer treatment system
Gresham Smith begins designing four proton therapy vaults for a Flint, Mich., medical center.
Gresham Smith | Nov 21, 2022
An inside look at the airport industry's plan to develop a digital twin guidebook
Zoë Fisher, AIA explores how design strategies are changing the way we deliver and design projects in the post-pandemic world.
Gresham Smith | Feb 13, 2022
Helping maximize project dollars: Utility coordination 101
In this post, I take a look at the utility coordination services our Transportation group offers to our clients in an attempt to minimize delays and avoid unforeseen costs.
Gresham Smith | May 7, 2021
Private practice: Designing healthcare spaces that promote patient privacy
If a facility violates HIPAA rules, the penalty can be costly to both their reputation and wallet, with fines up to $250,000 depending on the severity.
Gresham Smith | Mar 4, 2021
Behavior mapping: Taking care of the caregivers through technology
Research suggests that the built environment may help reduce burnout.