The new Parkland Hospital is big. Check out the numbers: 862 private adult beds and 96 neonatal ICU beds. More than two million sf of space, and $1.27 billion in construction cost. Ten thousand employees. A hundred fifty minority/women/small business contractors. Five million man-hours in trades labor.
When it opens August 20, 30,000 visitors—speaking 77 languages—will stream through the new Parkland hospital daily, 140,000 people will seek care in its ED annually, and 16,000 babies will be born there every year.
As the largest public healthcare project in the country to be built in one phase, Parkland hospital “will serve as a standard for public healthcare development into the future,” said Lou Saksen, Senior Vice President for New Parkland Construction.
PROJECT SUMMARY
GOLD AWARD
Parkland Hospital
Dallas, TexasBUILDING TEAM
Submitting firm: HDR
Owner: Parkland Health & Hospital System
Architect, interior architect, master planner: HDR+Corgan Joint Venture
Programming consultant: Blue Cottage
Structural engineer: AG&E Structural Engenuity
MEP engineer: HDR
Civil engineer: Pacheco Koch
Electrical engineer (power): MEP Consulting Engineers, Inc.
CM: BARA (Balfour Beatty Construction, Austin Commercial, H.J. Russell & Company, and Azteca-Omega Group joint venture)GENERAL INFORMATION
Project size: 2.1 million sf
Construction cost: $1.27 billion
Construction time: October 2010 to October 2014
Delivery method: Collaborative project delivery (no contract)
MAKING THE COMPLEX SIMPLE
In 2008, Dallas County voters overwhelmingly approved a $747 million bond issue to replace the 1950s-era existing hospital. The design team of HDR+Corgan, a four-firm construction management group known as “BARA,” and programmer Blue Cottage were tasked with creating a master plan for the 64-acre medical campus and a building design for a LEED-NC 2009 Silver hospital. Ground was broken in May 2010; construction was completed last October.
What sounds like a relatively smooth execution belies the complexity of the project and the Herculean effort the Building Team made to make it seem easy.
Using what they called “collaborative project delivery”—an IPD with no contract—the team held visioning sessions to picture the future Parkland hospital from curbside to bedside. They brought in a consultant to coach them on teamwork. They co-located their workspace. They had estimators in place to make immediate evaluations of changes in costs. They set up a robust Patient & Family Advisory Council that had a real impact on program and design decisions.
They created three full-time “clinical liaison positions” staffed by veteran Parkland hospitial nurses, who acted as links to the medicine, surgery, and women’s services divisions. RNs “helped inform the entire design of the space,” said Kathy Harper, RN, MBA, EDAC, Parkland’s Director of Clinical Planning.
The team pulled out all the stops to solve a huge array of technical problems. They built mockups galore—a patient room, an OR, an NNICU room, a labor/delivery room—to gather feedback from hundreds of physicians, clinicians, and technicians. They prefabricated 750 bathroom units, 850 headboards, and three miles of MEP systems offsite.
When projections of ED use ballooned from a planned 100,000 visits a year to a possible 240,000, the team halted construction on the ED, redesigned it, and added a shelled bay of 12 exam rooms for future expansion.
When, in 2011, new hospital management asked for a “reexamination” of key design elements, the team enlarged ambulatory facilities on the main campus to meet anticipated demand. They reconfigured the radiology department into separate inpatient/outpatient units instead of a single unit as originally planned. They even redesigned the dietary kitchen so that patients could have 24-hour room service.
They standardized the ORs to allow for different types of equipment to be brought in, depending on the procedure. Conduits and cable trays were oversized. Floor-to-floor heights were bumped up to support future technologies.
According to Fred Cerise, MD, President/CEO, Parkland Health & Hospital System, “The legacy of this institution is cemented as an innovator in providing quality care for the medically underserved, as a leader in clinical expertise in specialties like burns and trauma, and as a pioneer of 21st-century transformational care processes.”
 A curvilinear garden with drought-resistant plantings helps fulfill the hospital’s objective to “put the park back in Parkland.” Public transportation to the hospital comes via the Dallas Area Rapid Transit Green Line and the new Parkland Station and Bus Transit Center. Patients and families access the parking facilities from the interior of the site; staff access parking from the perimeter.
A curvilinear garden with drought-resistant plantings helps fulfill the hospital’s objective to “put the park back in Parkland.” Public transportation to the hospital comes via the Dallas Area Rapid Transit Green Line and the new Parkland Station and Bus Transit Center. Patients and families access the parking facilities from the interior of the site; staff access parking from the perimeter.
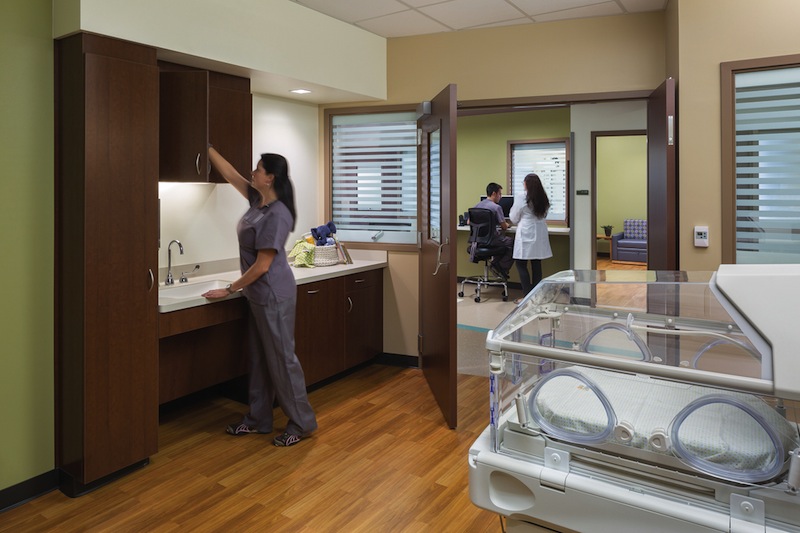 Evidence-based design and practices—exposure to natural light, decentralized nursing stations, healing gardens, noise reduction, soft lighting, etc.—play a significant role at Parkland. The neonatal ICU will be a test site for various EBD strategies, such as having an onsite pharmacy to reduce dosing errors. As a Pebble Project hospital, Parkland is engaged in multiple research projects, including wayfinding and reception-area seating arrangements.
Evidence-based design and practices—exposure to natural light, decentralized nursing stations, healing gardens, noise reduction, soft lighting, etc.—play a significant role at Parkland. The neonatal ICU will be a test site for various EBD strategies, such as having an onsite pharmacy to reduce dosing errors. As a Pebble Project hospital, Parkland is engaged in multiple research projects, including wayfinding and reception-area seating arrangements.
Related Stories
| Aug 29, 2022
Montana becomes first U.S. state to approve 3D printing in construction
Montana is the first U.S. state to give broad regulatory approval for 3D printing in building construction.
Architects | Apr 22, 2022
Top 10 green building projects for 2022
The American Institute of Architects' Committee on the Environment (COTE) has announced its COTE Top Ten Awards for significant achievements in advancing climate action.
Concrete Technology | Apr 19, 2022
SGH’s Applied Science & Research Center achieves ISO 17025 accreditation for concrete testing procedures
Simpson Gumpertz & Heger’s (SGH) Applied Science & Research Center recently received ISO/IEC17025 accreditation from the American Association for Laboratory Accreditation (A2LA) for several concrete testing methods.
2021 Building Team Awards | Jan 14, 2022
First public-private partnership project in Veterans Administration history saves $34 million in costs
LEO A DALY and McCarthy Building Companies head the project team for the Omaha VA Ambulatory Care Center in BD+C’s 2021 Building Team Awards.
Building Team Awards | Dec 8, 2021
A performing arts center celebrates a legendary rocker and his birthplace
Buddy Holly Hall in Texas receives BD+C’s Silver Building Team Award.
Building Team Awards | Dec 7, 2021
A rapid response to a health emergency
Baptist Hospital of Miami’s 233-bed Hope Tower receives BD+C’s Bronze Building Team Award
Building Team Awards | Dec 3, 2021
Putting science on display, thanks to a design-build approach
UC Riverside’s Plant Growth Environments Facility receives BD+C’s Bronze Building Team Award.
Building Team Awards | Dec 2, 2021
An academic ‘precinct’ brings arts and sciences together
Wofford College’s Chandler Center for Environmental Studies receives BD+C’s Silver Building Team Award.
Building Team Awards | Dec 1, 2021
Denver sets the bar for water reclamation and reuse
A new administration building for the city’s water utility company scores Platinum in BD+C’s 2021 Building Team Awards.
2021 Building Team Awards | Nov 17, 2021
Caltech's new neuroscience building unites scientists, engineers to master the human brain
The Tianqiao and Chrissy Chen Institute for Neuroscience at the California Institute of Technology in Pasadena wins a Gold Award in BD+C's 2021 Building Team Awards.